Tuberculosis: A Persistent Global Health Threat
Tuberculosis (TB) remains one of the world's deadliest infectious diseases, claiming over a million lives each year. TB is the deadliest infectious disease known today, claiming more lives than COVID-19. TB is caused by the bacterium Mycobacterium tuberculosis. TB spreads through the air when infected people breathe, cough, sneeze, or speak. Standard drug treatments exist, and drug treatment regimens can last 12 months or longer and involve multiple drugs taken daily.
This long duration leads to poor adherence as some infected patients do not take their drugs every day, all patients experience prolonged side effects from the drugs, and, most alarmingly, the rise of drug-resistant strains of TB is a problem even for patients who take drugs as directed. Because of how long the treatment lasts and the emergence of drug-resistant strains, serious burdens are placed on hospitals and doctors’ offices to contain the deadly disease in high-burden countries such as those in Africa and Southeast Asia.
The Growing Challenge of Drug-Resistant TB
Drug resistance occurs when TB bacteria mutate and survive exposure to antibiotics that once killed them, for example, because patients are not taking the drugs regularly as directed. Multidrug-resistant TB resists the two most powerful first-line drugs, while extensively drug-resistant forms add resistance to key second-line options.
These resistant infections require longer, more toxic, and more costly regimens, sometimes up to two years, with lower success rates. As resistance spreads globally, the need for new drugs that work differently from existing ones has become urgent.
Targeting a Critical Weakness: The DprE1 Protein
Scientists are now targeting vulnerabilities in the TB bacterium that current treatments overlook. One of the most promising targets is a protein called DprE1 (decaprenylphosphoryl-β-D-ribose 2'-epimerase).
DprE1 plays a vital role in building the bacterium's tough outer cell wall, a protective layer made of complex fats and complex sugars. These components help TB survive inside immune cells and resist many antibiotics. Blocking DprE1 kills TB bacteria, weakening the cell wall until the bacterium bursts and dies, even in resistant strains, since many older drugs target different pathways.
DprE1 is especially attractive because it is located on the outer surface of the cell membrane, making it easier for drugs to reach without crossing into the bacterium's interior. Genetic studies also show that without functional DprE1, TB bacteria cannot survive.
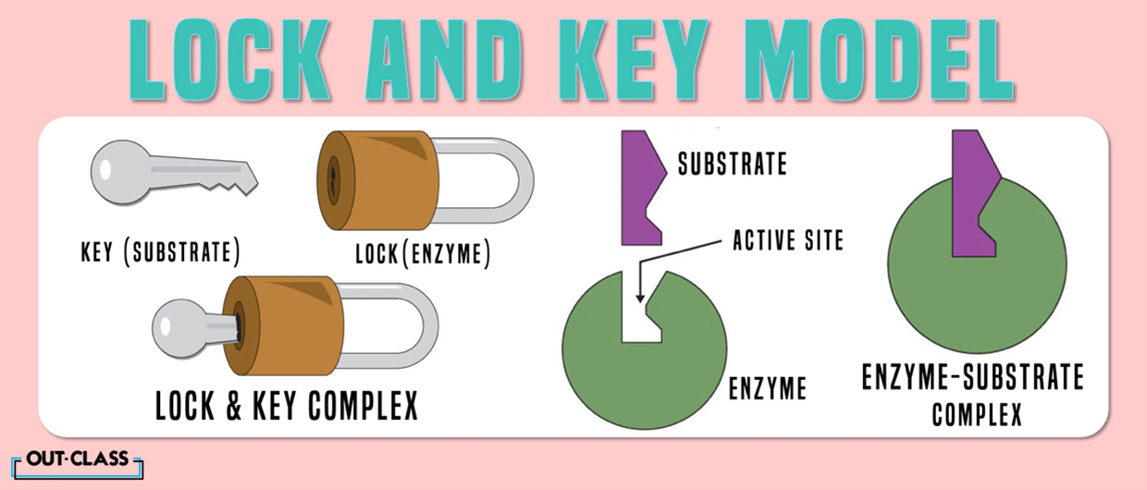
Importantly, humans do not have a direct equivalent of DprE1, which reduces the risk of harmful side effects. In simple terms, the DprE1 protein acts like a lock, and the drug acts like the key, specifically designed to disable the bacterial system without interfering with human proteins.
Accelerating Drug Discovery with DNA-Encoded Libraries
To accelerate the discovery of new drug candidates, researchers are using advanced screening technologies such as DNA-encoded libraries (DELs).
Traditional drug screening tests compounds one by one or in small groups, which makes the process slow and expensive. DEL technology changes this by creating enormous libraries of molecules—sometimes billions—each attached to a unique DNA barcode that records the molecule’s chemical structure.
During a DEL screen, the entire library is exposed to a target protein such as DprE1. Molecules that bind to the protein are captured while the others are washed away. Scientists then sequence the DNA barcodes to identify which compounds successfully bound to the target.
This high-throughput method dramatically speeds up drug discovery. DELs have already produced promising TB inhibitors targeting several bacterial proteins, demonstrating strong potential in antibacterial research.
A New Era in Tuberculosis Drug Development
Combining validated targets such as DprE1 with powerful screening technologies like DNA-encoded libraries represents a new era in TB drug discovery.
Recent research pipelines show encouraging progress. In addition to DprE1 inhibitors, other novel compounds are entering clinical trials and may shorten treatment durations when combined with existing drugs. The global TB pipeline now includes dozens of potential drug candidates, with more entering testing each year.
The Future of TB Treatment
These advances aim to deliver shorter, simpler, and safer treatment regimens that remain effective against drug-resistant TB strains. Such therapies could significantly improve patient adherence and treatment outcomes worldwide.
Challenges still remain, including funding gaps and the need for combination therapies to prevent new resistance from emerging. However, the outlook is increasingly hopeful.
By targeting bacterial weaknesses such as DprE1 and harnessing innovative technologies like DNA-encoded libraries, scientists are steadily moving closer to the next generation of TB medicines—treatments that could transform care and ultimately save millions of lives.



Discussion