Imagine deploying a therapy that does not just treat disease, but actively enlists the body's own immune defenders to do the work. This is the principle behind a growing field that designs drug carriers specifically to be recognized, internalized, and processed by antigen-presenting cells (APCs). These specialized immune cells, including dendritic cells, macrophages, and M cells, serve as the immune system's command centers, bridging innate threat detection and adaptive responses capable of targeting specific pathogens. Learning to engineer particles that speak the language of APCs is reshaping how researchers approach vaccines, immunotherapies, and treatments for respiratory infections.
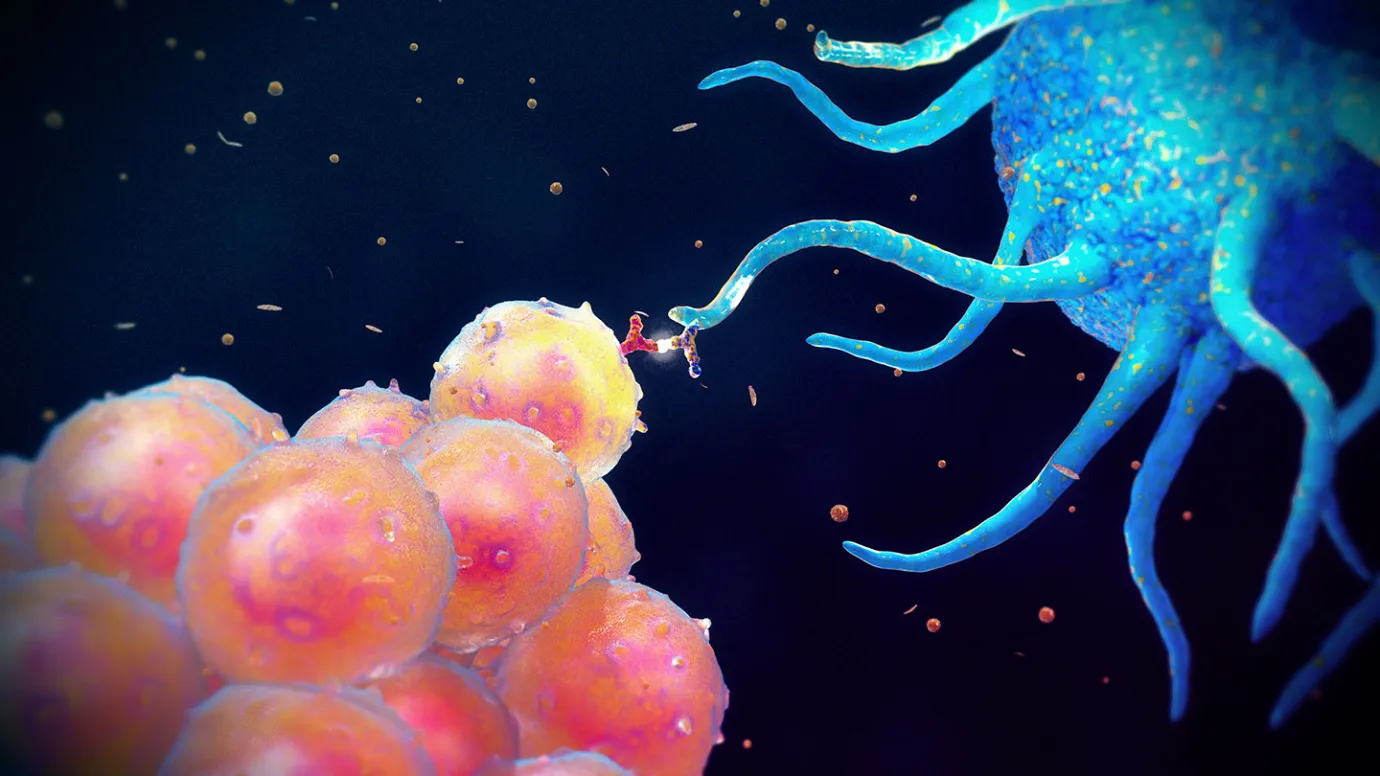
The Commanders of Immune Response
APCs are not a single cell type. They form a diverse network united by one defining ability: to capture foreign material, process it, and present fragments to T cells through major histocompatibility complex (MHC) molecules. This presentation is the ignition point of adaptive immunity.
Dendritic cells (DCs) are considered the most potent APCs for initiating immune responses. Distributed across mucosal tissues and circulating in the bloodstream, DCs carry pattern recognition receptors, including Toll-like receptors and C-type lectin receptors, which detect pathogen-associated molecular patterns (Banchereau et al., 2000). Once activated, they migrate to lymph nodes and orchestrate both cellular and humoral immunity.
Alveolar macrophages represent the first phagocytic line of defense in the lungs. While less specialized than DCs at antigen presentation, they are highly efficient at particle engulfment. Studies show that phagocytosis of micron-sized particles can begin within the first 2-3 hours of deposition (Geiser, 2010). Their abundance in the alveolar space makes them a priority target for inhaled formulations.
M cells represent a third route. These specialized epithelial cells, found in the Peyer's patches of the gut and in respiratory mucosa, sample luminal contents and transport antigens to underlying immune cells (Dillon & Lo, 2019). Their role in non-invasive vaccination strategies is attracting growing research attention. Together, these populations form an interconnected surveillance network, and drug delivery science is learning how to interface with each one.
Particle Design as a Biological Language
Recognizing that APCs are present throughout the body is only the first step. The challenge is designing particles these cells will recognize, internalize, and respond to in a controlled, beneficial way.
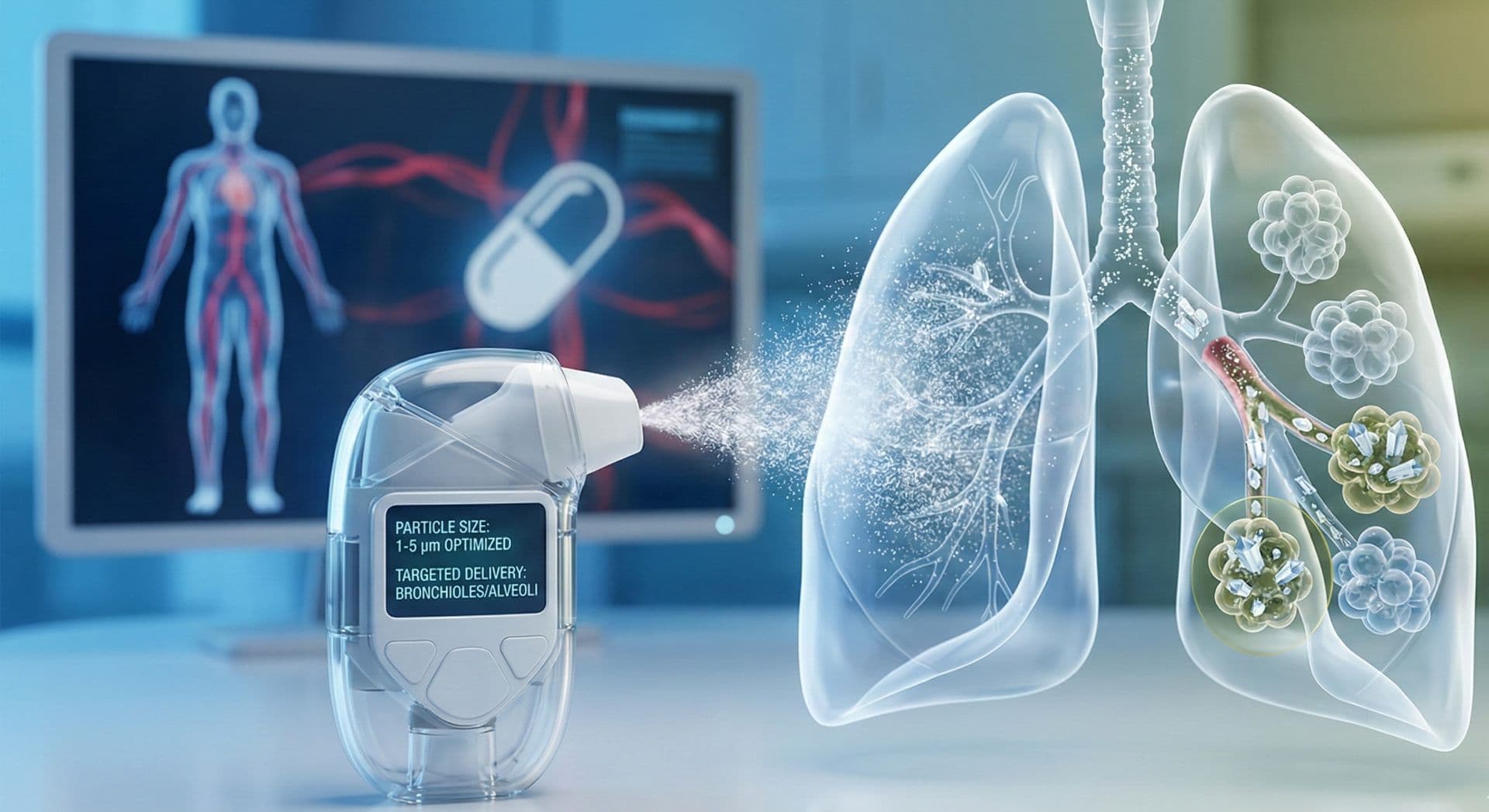
Particle size is the most studied variable. Particles of 0.5 to 5 micrometers are typically phagocytosed by macrophages, mimicking the size of bacteria and triggering humoral immune responses. Smaller particles, around 20-200 nm, tend to be taken up by DCs, favoring cellular immunity (De Temmerman et al., 2011). This size-dependent behavior gives formulators a tunable parameter for steering immune outcomes.
Shape is equally consequential. Irregularly shaped particles with high surface curvature can activate inflammasome pathways and enhance immune recognition (Baranov et al., 2020). Collapsed, convoluted morphologies, such as those produced during spray-drying, are not merely manufacturing byproducts. They can actively influence how APCs engage with the particle surface.
Surface chemistry enables highly specific targeting. C-type lectin receptors, including the mannose receptor (CD206), recognize carbohydrate residues such as mannose and galactose. Natural polymers bearing these sugars, including locust bean gum, a galactomannan derived from carob tree seeds, exploit these receptors to achieve preferential APC uptake (Rodrigues & Grenha, 2015). In recent work, 70-90% of M2-polarized macrophages successfully internalized galactomannan-based microparticles after just two hours of exposure (Pinto da Silva et al., 2025).
Triggering the Right Downstream Response
Targeting APCs is not an end in itself. Once internalized, the delivered cargo must trigger the right downstream response. Particle-associated antigens are processed far more efficiently by APCs than soluble ones, generating stronger MHC-II presentation and more robust T and B cell activation (De Temmerman et al., 2011).
For pulmonary immunization, this translates into a tangible advantage. Delivering antigens directly to the lung mucosa, where DCs, macrophages, and M cells converge in high density, can elicit both local secretory IgA responses and systemic IgG production (Lavelle & Ward, 2022). Secretory IgA is particularly valuable as it neutralizes pathogens at the mucosal surface before infection can establish.
Sustained antigen release extends this effect. When antigens are distributed both on particle surfaces and within the carrier matrix, a biphasic release pattern emerges, combining immediate immune activation with prolonged antigen availability. This sustained presentation more faithfully mimics the kinetics of natural infection, providing a stronger and more durable signal to the immune system (Ou, 2022).
Why This Matters Beyond the Laboratory
APC-targeted drug delivery carries implications well beyond experimental models. For vaccine development, this approach offers a path to non-invasive, needle-free immunization that generates mucosal protection, something traditional injected vaccines consistently fail to provide. For respiratory infections, where pathogens first encounter the immune system at mucosal surfaces, this distinction is critical.
For antimicrobial resistance, APC-targeting offers a strategic alternative: therapies that strengthen host defenses rather than attacking pathogens directly, reducing the selective pressure that fuels resistance. As drug-resistant infections rise globally, approaches rooted in the body's own immune architecture may prove among the most durable available.
Conclusion
Antigen-presenting cells are not passive targets. They are active biological partners whose behavior can be shaped by deliberate particle design, material selection, and site of deposition. As researchers refine the language of size, shape, and surface chemistry, the possibility of truly intelligent therapies grows clearer. Pulmonary delivery, mucosal vaccination, and immunomodulation are converging on a shared principle: the most effective medicines may ultimately be those that teach the immune system to act, rather than acting in its place.


Discussion