Introduction
Environmental endocrine disruptors (EEDs) are natural and synthetic chemicals that interfere with endocrine system function by altering hormone synthesis, transport, metabolism, and receptor binding. These compounds are widely distributed in the environment and consumer products, resulting in continuous, low-level human exposure. Unlike classical toxicants, EEDs can exert biological effects at environmentally relevant concentrations, particularly during sensitive developmental periods such as prenatal and early postnatal life (Encarnação et al., 2019; Rubin, 2011).
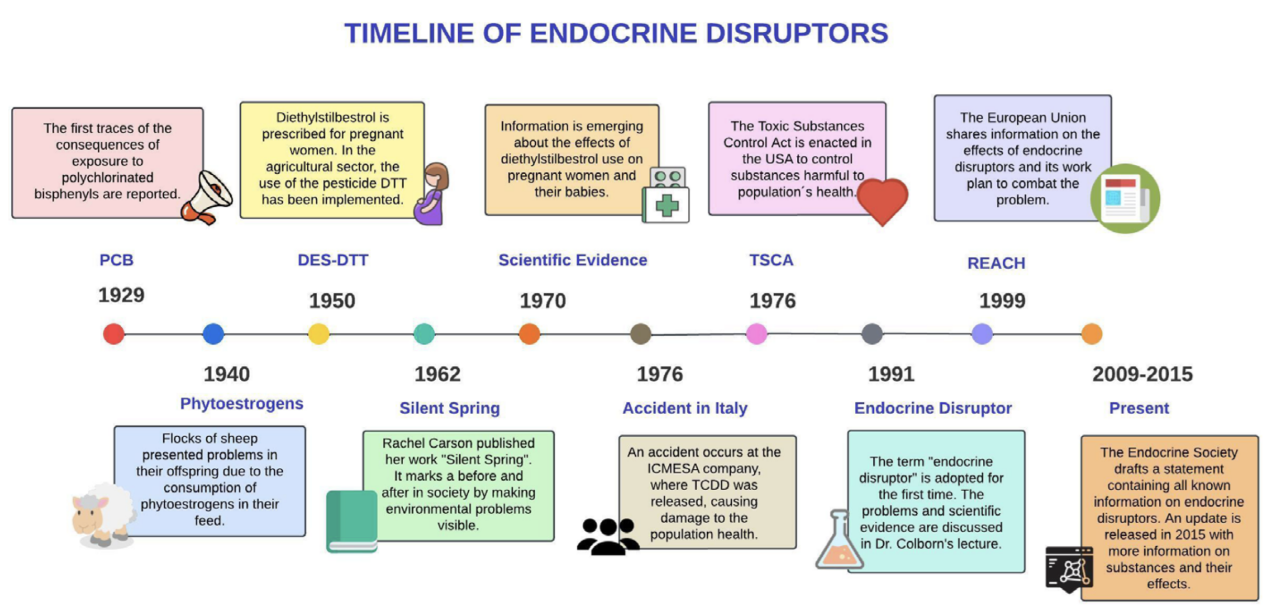
How Endocrine Disruptors Act
At the molecular level, EEDs disrupt endocrine signaling through several established mechanisms. Many compounds function as agonists or antagonists of estrogen, androgen, and thyroid hormone receptors, thereby modifying gene transcription and downstream physiological pathways. Others interfere with endocrine regulation by altering key enzymes involved in hormone biosynthesis and metabolism, including aromatase and deiodinases.
In addition, some EEDs are associated with epigenetic modifications, such as changes in DNA methylation and chromatin structure, which can lead to persistent alterations in gene expression and, in some cases, transgenerational biological effects (Rubin, 2011; Skinner et al., 2013; Encarnação et al., 2019).
Common Sources of Exposure in Daily Life
Every day exposure to endocrine disruptors occurs through multiple consumer and environmental pathways, including:
Plastics and food-contact materials: Migration of bisphenols and phthalates into food and beverages
Personal care and household products: Preservatives, fragrances, and additives with endocrine-disrupting properties
Environmental contamination: Agricultural chemicals and industrial pollutants affecting water, soil, and dietary sources (Encarnação et al., 2019; Kumar et al., 2020)
These overlapping exposure routes often result in complex chemical mixtures entering the human body, complicating conventional risk assessment approaches.
Health Implications Across the Lifespan
EED exposure has been associated with a range of biological and clinical outcomes. Reproductive and developmental effects include altered pubertal timing, impaired fertility, and increased susceptibility to hormone-sensitive cancers, particularly when exposure occurs during early life stages (Encarnação et al., 2019). Beyond these classical endocrine outcomes, EEDs are increasingly recognized as contributors to metabolic dysfunction. Evidence indicates that several endocrine disruptors can interfere with insulin signaling, promote chronic low-grade inflammation, and alter adipose tissue regulation, thereby increasing the risk of obesity, insulin resistance, and type 2 diabetes (Kumar et al., 2020; Dagar et al., 2023). Disruption of thyroid hormone pathways has also been linked to neurodevelopmental and cognitive effects, reflecting the critical role of thyroid hormones in brain development (Encarnação et al., 2019).
Regulatory and Scientific Challenges
A key challenge in managing endocrine disruptors lies in the limitations of traditional toxicological models. High-dose testing and assumptions of linear dose response relationships may not adequately capture the low-dose and non-monotonic effects reported for many EEDs. Additionally, real-world exposure typically involves chemical mixturesrather than individual compounds, complicating hazard identification and regulatory decision-making (Encarnação et al., 2019; Kumar et al., 2020). From a research perspective, there is a growing need for long-term and multigenerational studies to better understand persistent and heritable effects, particularly those mediated by epigenetic mechanisms (Skinner et al., 2013).
Conclusion
Environmental endocrine disruptors represent a widespread and scientifically complex public health concern. Evidence from molecular, experimental, and epidemiological studies demonstrates their ability to interfere with hormonal regulation and contribute to reproductive, metabolic, and neurodevelopmental disorders across the lifespan. Addressing these challenges will require improved risk assessment strategies, stronger regulatory frameworks, and continued integration of mechanistic and population-based research to inform evidence-driven public health policies (Encarnação et al., 2019; Kumar et al., 2020; Dagar et al., 2023).



Discussion