The conventional model of medical diagnosis certainly depends on the appearance of the clinical symptoms, a framework that inevitably delays involvement until disease processes are well-established. Many illnesses, particularly metabolic, cardiovascular, neurological, and immune-mediated ailments, begin with minor molecular or physiological changes that remain undetected with standard clinical assessment. Recent advances in artificial intelligence have initiated a profound shift in this prototype. AI-driven systems are designed to detect the earliest biological deviations from homeostasis, providing a window into the pre-symptomatic stage of disease development, rather than reacting to disease after it is clinically diagnosed. This approach has the potential not only to enrich diagnostic precision but also to improve healthcare as a proactive, prophetic, and personalised discipline. AI's advancement in early illness diagnosis depends on its ability to identify subtle patterns in large, complex datasets. Human physiology generates continuous streams of data, ranging from genetic and proteomic profiles to electrocardiographic signatures, endocrine and metabolic biomarkers, gait dynamics, voice characteristics, and behavioural characteristics. On their own, these data points might not appear clinically significant. However, AI algorithms trained on huge datasets may identify complex relationships between these factors, showing early problematic indications that are invisible to humans as symptoms. Machine-learning algorithms, particularly deep learning designs, could provide extremely accurate predictions regarding the progression of an illness by analysing non-linear links in such data.
Cardiovascular medicine is one of those fields where early AI-driven prediction has shown strong therapeutic potential. Structural and electrophysiological complications in cardiovascular diseases can develop silently long before clear symptoms like arrhythmias or chest pain. According to research, neural network prototypes usually extract prognostic
information from seemingly normal electrocardiograms to identify individuals who are more likely to develop atrial fibrillation months in advance. Similarly, it has been found that by detecting tiny microvascular changes associated with atherosclerosis and hypertension, AI analysis of retinal fundus pictures can predict cardiovascular risk. These findings show how AI could transform routine clinical data into predictive biomarkers, potentially preventing tragic
cardiac episodes and enabling earlier intervention. Metabolic diseases are another strong example of the application of AI in pre-symptomatic evaluation. Metabolic flexibility, insulin sensitivity, and glucose levels gradually decrease during the extensive subclinical phase of type 2 diabetes. AI models that integrate information from genetics, dietary habits, microbiome composition, and continuous monitoring of glucose have shown the ability to detect metabolic dysregulation years before conventional diagnostic criteria are satisfied. These models could describe early fluctuations in insulin receptivity or glucose variability that would not be detected through normal laboratory tests. This provides a chance for timely lifestyle changes or therapies that could prevent or significantly defer the beginning of diseases.
The usage of AI to detect early physiological changes became particularly clear and popular during the COVID-19 pandemic. Wearable sensors, such as fitness trackers and smartwatches, produced continuous data on body temperature, respiration rate, heart rate, andsleep schedule. 48–72 hours before the onset of symptoms, AI models are trained on these data, and theycand
recognize physiological markers associated with the disease. It demonstrates that everyday gadgets can be used for population-wide, passive disease surveillance. This idea could be very
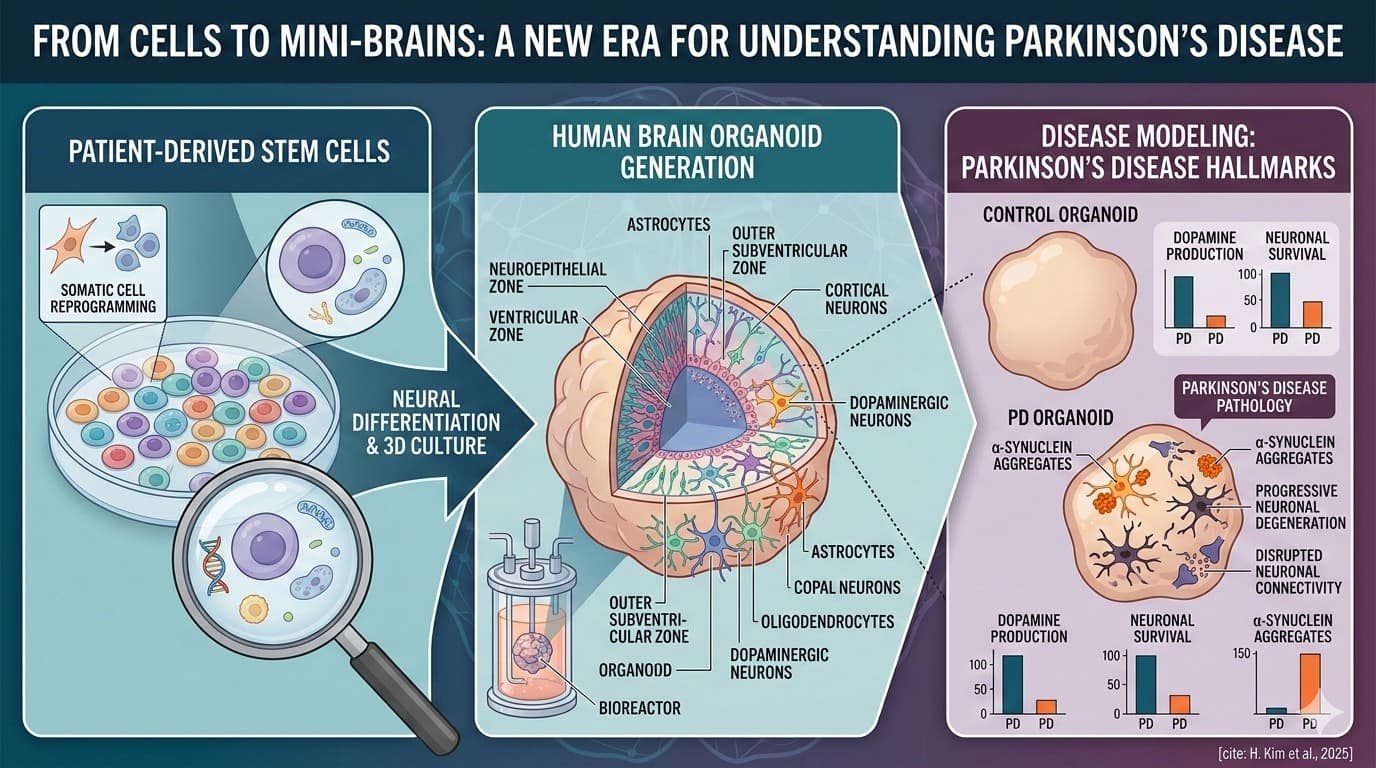
AI algorithms that examine digital behaviour, advanced search trends, and online communication patterns can identify new disease clusters before authorized case counts do, providing a powerful tool for public health preparedness on a larger epidemiological scale. Neurological illnesses are yet another field where AI plays a significant role in early disease prediction. Several neurodegenerative disorders, such as Parkinson's and Alzheimer's, begin with slight alterations in brain function long before there is any significant or observable acute impairment. AI-driven analysis of speech patterns, motor behaviour, respiration signals, and brain imaging analysis has shown remarkable precision in identifying patients in the prodromal phases of these disorders. Changes in speech amplitude variation and articulation, for instance, have been found to indicate early Parkinsonian illness, and natural language processing algorithms can detect linguistic deterioration suggestive of preclinical Alzheimer's disease. These results highlight that early neurological changes may be evaluated long before conventional tests detect them, provided the appropriate computational techniques are put into action.
AI can identify behavioural and physiological indicators linked to stress-related disorders like anxiety and depression, making mental health prediction aanemerging field. Constant observation of a person's vocal tone, daily activity profiles, sleep cycles, and digital interaction patterns could identify early from normal that might point to psychological discomfort. Early detection may allow for more prompt support and slow the spread of mental health crises, even though privacy ethics are especially delicate in this area. Despite its revolutionary assurance, AI-driven early disease prediction faces numerous challenges. The reliability of prediction models is strongly influenced by the quality and diversity of training datasets. Bias in the underlying data may lead to differences in performance prediction amongstpopulationss, which presents ethical and medical challenges. Further, to avoid incorrect diagnosis and needless patient anxiety, caution must be used when evaluating risk assessments. Ensuring data privacy, creating transparent model interpretability, and correctly integrating AI into healthcare, specifically intodecision-making frameworksk ise still necessary for implementation.
However, the path of AI-powered healthcare is more about anticipation than reaction. Artificial Intelligence (AI) may identify disorders at their earliest genetic or physiological roots, perhaps halting harmful progression before a patient ever shows ysymptoms This paradigm would reduce the long-term burden on healthcare systems in addition to boosting individual health outcomes. An era where preserving health comes before curingillnesss may be steered in by early ailment detection through AI as research advances and computational models get more complex and tedious.



Discussion